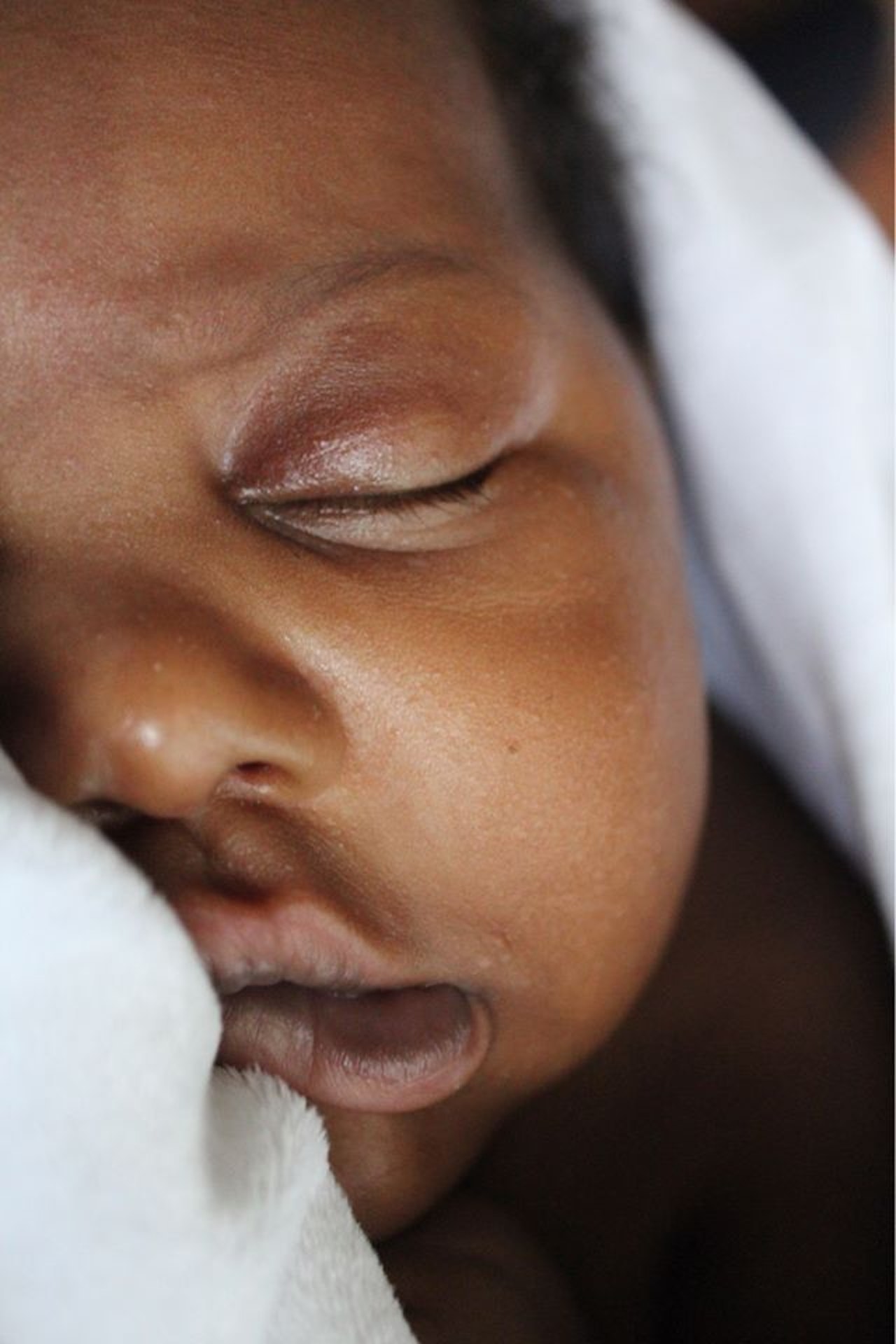
Jaundice, a sign of elevated bilirubin levels, is common during the first weeks of life, especially among preterm newborns. Bilirubin, a product from the normal breakdown of red blood cells, is elevated in newborns for several reasons:
- Newborns have a higher rate of bilirubin production due to the shorter lifespan of red blood cells and higher red blood cell concentration compared to adults.
- Newborns have immature liver function, leading to slower metabolism of bilirubin.
- Newborns may have a delay in passage of meconium, leading to increased reabsorption of bilirubin in the intestines.
- In most newborns, jaundice is termed “physiologic jaundice” and is considered harmless.
What is the difference between suboptimal intake jaundice and breast milk jaundice?
Suboptimal intake jaundice, also called breastfeeding jaundice, most often occurs in the first week of life when breastfeeding is being established. Newborns may not receive optimal milk intake, which leads to elevated bilirubin levels due to increased reabsorption of bilirubin in the intestines. Inadequate milk intake also delays the passage of meconium, which contains large amounts of bilirubin that is then transferred into the infant’s circulation. In most cases breastfeeding can, and should, continue. More feedings can reduce the risk of jaundice.
Breast milk jaundice most often occurs in the second or later weeks of life and can continue for several weeks. While the exact mechanism leading to breast milk jaundice is unknown, it is believed that substances in the mother’s milk inhibit the ability of the infant’s liver to process bilirubin.
Phototherapy is a common treatment for jaundice. Other therapeutic options include temporary supplementation with donor human milk or infant formula, and rarely, temporary interruption of breastfeeding.
Source: CDC
Link: https://www.cdc.gov/breastfeeding/breastfeeding-special-circumstances/maternal-or-infant-illnesses/jaundice.html